How We Feel Pain
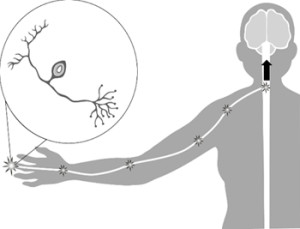 Pain is a complex physiological process. A pain message is transmitted to the brain by specialized nerve cells known as nociceptors, or pain receptors (pictured in the circle to the right). When pain receptors are stimulated by temperature, pressure or chemicals, they release neurotransmitters within the cells. Neurotransmitters are chemical ‘messengers’ in the nervous system that facilitate communication between nerve cells.
Pain is a complex physiological process. A pain message is transmitted to the brain by specialized nerve cells known as nociceptors, or pain receptors (pictured in the circle to the right). When pain receptors are stimulated by temperature, pressure or chemicals, they release neurotransmitters within the cells. Neurotransmitters are chemical ‘messengers’ in the nervous system that facilitate communication between nerve cells.
As seen in the diagram, these messengers transmit a pain signal from the pain receptor to the spinal cord, and then to the thalamus, a region of the brain. The thalamus then transmits the pain signal to other areas of the brain to be processed.
Once the brain has received and interpreted the pain message, it coordinates an appropriate response. The brain can send a signal back to the spinal cord and nerves to increase or decrease the severity of pain. For example, the brain can signal the release of natural painkillers known as endorphins. Alternately, the brain can direct the release of neurotransmitters that enhance pain or hormones that stimulate the immune system to respond to an injury. Recent research has shown that people possess differing amounts of these neurotransmitters, possibly explaining why some people experience pain more intensely than others. Furthermore, recent studies have found that genetic makeup can influence an individual’s sensitivity to pain.
Types of Pain
In general, pain is divided into two categories: acute and chronic. In an acute pain episode, pain receptors transmit information about an injury to the spinal cord and brain, leading you to protect the injured area. Examples of acute pain are burning yourself on the stove or stubbing your toe. This type of pain resolves once the injury heals. Sometimes, however, your body heals, but your brain continues to perceive the pain. Genetics, physiological mechanisms and even psychological factors may be involved in the transformation of acute to chronic pain. Trying to determine exactly how acute pain becomes chronic is one of the major challenges for researchers studying pain.
The majority of medical providers define chronic pain as pain that persists for at least three to six months, but some health care providers describe it as pain that endures beyond the body’s normal healing time. In some cases, chronic pain is due to an ongoing medical condition, such as arthritis or cancer, but in many cases, it doesn’t have an identifiable cause.
There is also a distinction between somatic, visceral and neuropathic pain. Somatic pain originates in the skin or musculoskeletal tissue and may be described as sharp, aching, throbbing, or gnawing, whereas visceral pain originates from an internal organ, e.g., stomach, and is usually described as deep and aching. Neuropathic pain results from damage to a peripheral nerve(s), the spinal cord or the brain, and is most often described as a burning or stabbing sensation.
Chronic pain can last for months or years, be constant or intermittent, and vary in severity over time. Because we associate pain with an injury, chronic pain sufferers tend to be perplexed and distressed about their condition.